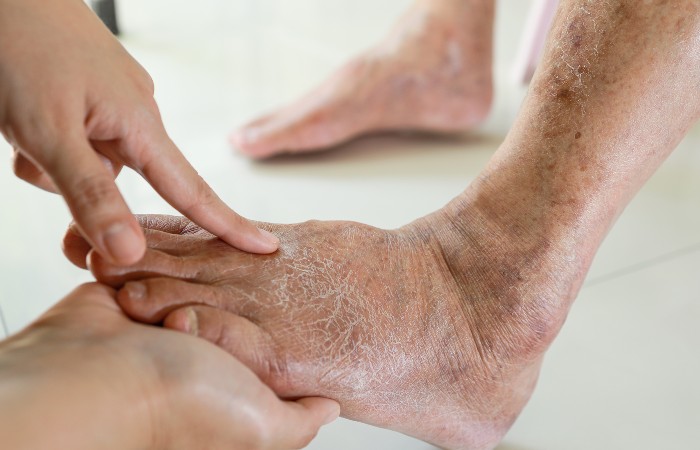
One step at a time
In Clinical
Follow this topic
Bookmark
Record learning outcomes
Pharmacists must be aware of how diabetes can affect the legs and feet, writes Victoria Goldman…
According to charity Diabetes UK, diabetes-related complications result in a lower limb amputation every 30 seconds. People with diabetes are up to 30 times more likely to have an amputation than those in the general population, and most diabetes-related amputations are caused by a foot ulcer failing to heal.
By keeping their blood glucose levels under control and having regular footcare check-ups, people with diabetes should be able to avoid complications.
When someone is first diagnosed with diabetes, they should be given information on optimal blood glucose management, the importance of daily foot care, what this involves, what to do if they experience any foot or leg problems, footwear advice and their risk of developing a foot problem in the future.
Annual foot checks are an important part of diabetes management and are free on the NHS. In Scotland, the foot check (or foot screening) may be less regular, depending on the person’s individual risk level for developing a serious foot problem.
Initial risk assessment
According to NICE guideline NG19, on ‘Diabetic foot problems: prevention and management’, reviewed in January 2023, everyone over the age of 12 years who is newly diagnosed with diabetes should have a footcare assessment to assess their risk of developing a diabetic foot problem.
If they are assessed as low risk, they will need to have an annual foot assessment alongside practising daily footcare – if they are unable to check or care for their own feet, they will need more-regular foot assessments.
If they are assessed as moderate to high risk, they will need a referral to the foot protection service to assess their feet, carry out checks and any necessary care (e.g. for foot ulcers) and assess the vascular status of their feet. The foot protection service is usually led by a specialist podiatrist and may be based in a health centre or GP clinic.
If someone has developed severe diabetes foot problems such as Charcot arthropathy (see below), they will be referred to the multidisciplinary foot care service, which is usually based at a hospital.
Common diabetes-related problems
Diabetes can affect the legs and feet in two ways. High blood glucose levels can reduce the nerve supply, which means patients may not experience pain or discomfort to warn them that a foot problem has occurred. High blood glucose levels can also affect the blood supply to the feet, reducing the circulation, delaying the healing of any cuts and sores and leading to cramping or pain.
If any foot or leg problems don’t get treated, these can lead to foot ulcers, infections and even amputations.
Diabetic foot ulcers affect around 10 percent of people with diabetes at some point in their lives. The ulcers are usually painless, under hard skin, and may be accompanied by pus, fluid build-up, redness and an unpleasant odour. Any dead, damaged or infected skin needs to be removed (called debridement) by a podiatrist and the wound dressings need to be changed by a healthcare professional.
Unnecessary standing and walking should be limited; a podiatrist may supply a pressure cast or other device or a special shoe to wear until the ulcer has healed. Any infection will need to be treated with antibiotics and any problems with blood flow will need to be addressed.
A diabetic foot infection can lead to a bone infection (osteomyelitis) if it remains untreated, so antibiotics must be taken as soon as possible. A small soft tissue or bone sample should be taken from the feet to assess which bacteria are causing the infection, and an X-ray may be necessary to check the extent of any damage.
Once a course of the appropriate antibiotics has been initiated, the infection should begin to clear up within one to two days.
Diabetic neuropathy is estimated to affect between up to one in four people with diabetes. It can cause burning, aching or shooting pains, as well as numbness. It may be treated with pain relief, tricyclic antidepressants, carbamazepine, gabapentin or topical capsaicin.
Charcot arthropathy is a serious condition caused by neuropathy and weakens the foot bones, leading to dislocations, fractures and changes in the shape of the foot. A Charcot foot may feel hot and painful and look swollen or red. Early treatment is essential to avoid complications, including amputation.
Anyone with suspected Charcot arthropathy must not put any weight on their feet until they have been seen by the multidisciplinary foot care service (this should be within two days). The treatment for Charcot arthropathy involves having a plaster cast fitted (usually for several months) to reduce the weight on the foot and ankle until the inflammation has settled.
Daily care
People with diabetes should be washing, drying and moisturising their legs and feet daily, as well as looking after their toenails. They should wear well-fitting comfortable footwear and check for signs of friction and other damage – they shouldn’t walk barefoot or use foot spas.
If their footwear is uncomfortable or causing foot problems, they should speak to a healthcare professional. Over-the-counter foot products, including medicinal products for foot problems, must be suitable for people with diabetes.
Checking for changes
If people with diabetes notice any foot or leg changes, they should seek medical advice straightaway. In particular, they should consult their GP if they experience:
- tingling sensations, pins and needles or numbness
- pain or burning or dull aching
- shiny, smooth skin on their feet
- hair loss on their legs and feet
- a loss of feeling in their legs or feet
- swollen feet
- reduce sweating on their feet
- wounds or sores that don’t heal
- cramp in their calves when resting or walking.
If they notice any changes in the colour or shape of their feet, have cold or hot feet, blisters or cuts that they can see but can’t feel, or a foul smell coming from an open wound – they should seek immediate advice from their local foot team.